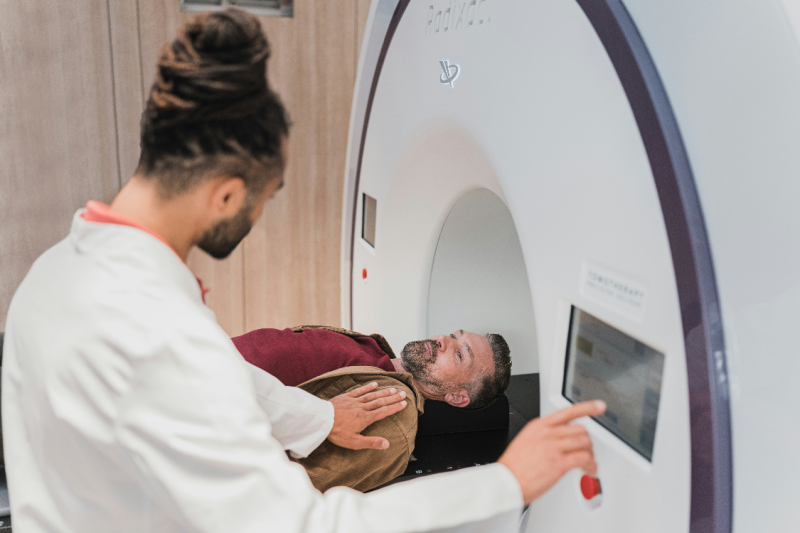
Radiology Information Systems and Picture Archiving And Communication Systems play a key role in modern clinical workflow and patient care. By organizing scheduling data and storing images in a central place they remove friction that used to slow clinicians down and frustrate patients.
These systems shorten the time from image capture to clinical decision and allow staff to focus more on care and less on paperwork. When implemented with clear rules and staff training the benefits become plain as day for both providers and patients.
For new staff or administrators, understanding how both systems fit together is critical to appreciating the full benefits of integration.
1. Streamlined Scheduling And Resource Allocation
A Radiology Information System centralizes appointment booking and matches available times with the right equipment and staff, which reduces idle scanner time and long patient queues. Clear calendar views and shared access let front desk staff and technologists coordinate without repeated phone calls or going back and forth across departments.
Automated checks in the workflow detect patient prep needs such as fasting or contrast screening and flag cases that need extra time, so the schedule reflects real world demands. This kind of planning helps clinics hit the ground running each morning rather than scrambling to catch up.
When exam orders arrive from other units the system can prioritize based on urgency and clinical context, making it easier to route cases to the right modality. That triage reduces pressure on peak hours and spreads workload more evenly over the day, which keeps staff energy up and reduces overtime.
A consistent scheduling flow also cuts the number of missed or duplicate appointments and lowers the need for last minute reschedules. Patients notice shorter waits and staff notice fewer fire drills when everyone follows a stable plan.
2. Faster Image Access And Reporting
A Picture Archiving And Communication System stores images in a searchable archive and delivers them to clinicians without physical media or long transmission delays. Radiologists can pull up prior studies next to new images and write reports with the full clinical history at hand, which speeds interpretation and supports clearer diagnosis.
Remote reading is practical when bandwidth allows, so subspecialists can help out across sites without being tied to a single reading room. When reports and images travel together the care team can act faster on results that matter most.
Integrated reporting tools help radiologists produce consistent reports with structured sections for findings and impressions, which reduces follow up queries from referring doctors. Templates and voice recognition can speed documentation while preserving nuance where needed, so reports are both quick and clinically useful.
Faster report turnaround closes the gap between test and treatment, which can be critical for time sensitive conditions. In practice that translates to fewer delays in starting therapy and less patient anxiety while waiting.
3. Reduced Redundancy And Improved Data Consistency

When RIS and PACS share a common patient identifier and study metadata the risk of duplicate imaging falls dramatically. Instead of ordering a repeat CT because prior films are missing a clinician can retrieve the prior exam and compare side by side, avoiding extra radiation and cost.
Consistent tagging of studies with procedure codes and clinical notes means downstream systems such as electronic medical records pull the right files automatically. That single source of truth reduces the paperwork load and cuts the number of times staff must chase missing information.
Structured data makes audits and billing more accurate because exam details are recorded in a predictable way rather than scattered across free text notes. Fewer discrepancies mean fewer claim denials and less time spent reconciling records at the business office.
From a clinical safety standpoint consistent data reduces the chance that a wrong exam gets matched to the wrong patient. In short, good data hygiene keeps the whole machine running more smoothly.
4. Better Collaboration Among Care Teams
Shared access to images and reports makes multidisciplinary discussion easier and more productive when teams meet to plan care. Clinicians in different departments can annotate images, leave notes, and flag studies for follow up without printing films or shipping disks.
When everyone can see the same timeline for a patient the care plan becomes clearer and handoffs carry less risk of miscommunication. That cooperative flow helps the whole team keep the ball rolling from admission through discharge.
Teleconsultation becomes practical for small hospitals that need remote specialist input, which widens access to expertise without moving patients. Surgeons, oncologists, and emergency clinicians can view relevant imaging at the bedside and make decisions quickly, which improves throughput in busy units.
Shared annotations and threaded discussions tied to specific studies reduce the need for repeat explanations and speed consensus. In urgent cases those saved minutes can be very meaningful.
5. Analytics Driven Operational Improvements
Logs and usage records from RIS and PACS reveal patterns that managers can use to tune operations and staffing. For example data on peak exam times and modality bottlenecks can guide schedule changes or capital planning for additional machines.
Predictive models built from historical queues and exam durations can suggest more realistic appointment lengths so schedule overruns become rarer. When administrators have hard numbers at hand they can make targeted changes rather than guesswork.
Quality metrics such as report turnaround times and repeat exam rates are simpler to track with centralized systems, and those metrics point to training needs or process fixes. Continuous monitoring helps teams test small changes and see measurable effects, which keeps improvement efforts focused and practical.
A culture that uses data to guide decisions tends to respond faster to new pressures and patient volumes. That practical approach brings steady gains in efficiency rather than sudden upheaval.